Chest pain naturally causes concern, especially when heart disease rates continue to rise. For people with asthma, this anxiety intensifies. So, the question arises, “Would asthma cause chest pain? Yes, it can.
However, not every kind of chest pain means heart trouble. Sometimes it is simply a result of short-term breathing difficulty or muscle strain from coughing. But if the pain persists and you feel unusual for days, it could be a sign of something more serious and should not be ignored.
This guide will help you understand the connection between asthma, chest pain, and heart diseases. It will also talk about when is the right time to seek medical advice.
Does Asthma Cause Chest Pain?
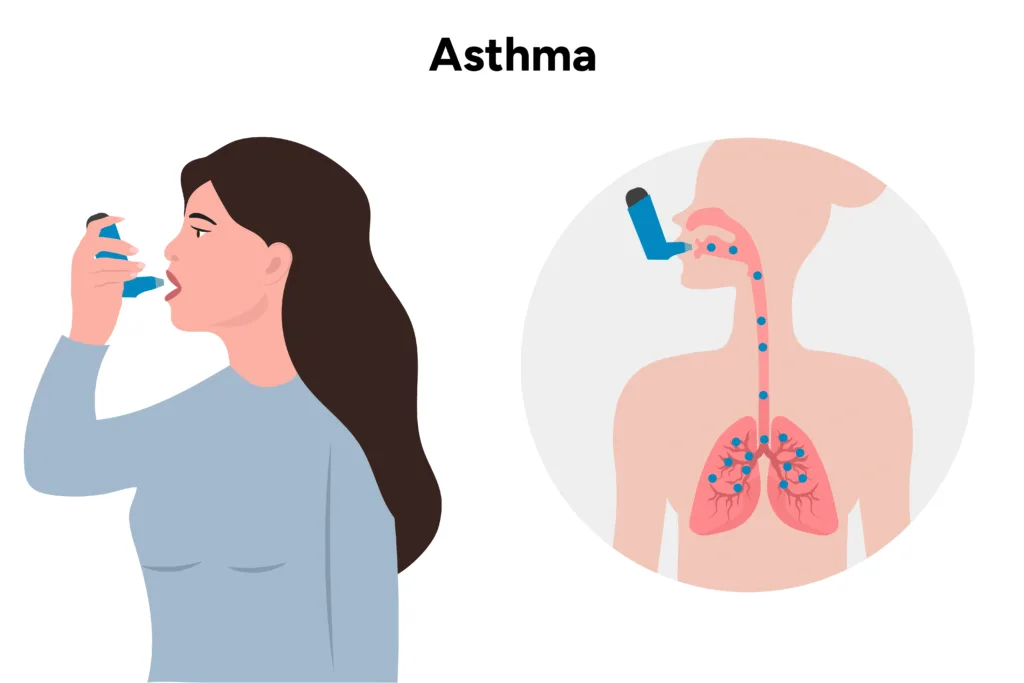
Asthma happens when the airways in your lungs become swollen and tight. This makes it harder for air to move in and out. The swelling and tightness also make chest muscles work extra hard to help you breathe. This effort can create soreness and tightness across the chest.
You might feel heavy pressure in your chest, especially during or after an asthma attack. The more severe the flare-up, the more your chest may hurt. Some people describe it as a sharp or pressing pain like their chest is wrapped too tightly.
Sometimes, this pain can show up even when you are not wheezing. Simple factors like cold air, smoke, or physical activity can make it worse. People who have allergies may also experience chest discomfort more often. It is because allergies cause chest discomfort by making the airways extra sensitive and easily irritated.
Why Chest Tightness Happens During Asthma

Chest tightness is one of the most common symptoms of asthma. When your airways get narrow, the lungs have to work harder to pull in oxygen. This strain can make your chest feel like it is being squeezed from the inside.
Here is what happens during an attack:
- The airway walls swell and inflame
- The muscles around them tighten
- Thick mucus builds up that blocks airflow
As a result, you feel pressure and pain in the chest, making breathing painful. Additionally, you may also feel breathlessness in asthma, especially when lying down or after light activity. For some, there is also a warm and stinging sensation which is often described as asthma burning in the chest.
Recognizing Chest Pain Symptoms Caused by Asthma
Chest pain from asthma feels different for everyone. But there are a few common signs that most asthma patients are likely to experience:
- A tight or heavy feeling in the center of your chest
- Pain that worsens when you cough, talk, or breathe deeply
- Wheezing and shortness of breath along with the pain
- Soreness in your chest muscles after breathing hard for a long time
If these signs appear often, your asthma may not be under control. But at this point, the good news is that your provider can adjust treatment and still help you learn how to relieve chest pain from asthma.
Sometimes, resting in a calm environment and using prescribed inhalers brings relief within minutes. If it does not, seek professional assistance.
Can Asthma Affect Your Heart Too?
Asthma mainly targets the lungs, but the effects do not stop there. When your oxygen levels drop, your heart has to pump harder to supply the body. Over time, this extra strain can lead to asthma heart problems.
Constant inflammation in the airways can affect blood vessels too. Although asthma alone does not directly cause heart attacks, it can raise the chances in extreme cases, such as when oxygen levels drop during severe asthma attacks.
In short, asthma can cause heart attacks, especially if your symptoms remain uncontrolled. Managing your asthma well helps protect both your lungs and heart.
When Asthma Chest Pain Feels Like a Heart Problem
Chest pain from asthma can feel alarmingly similar to pain from the heart. Both cause tightness, pressure, or shortness of breath. That’s why it is easy to mix up an asthma attack and heart attack.
A few key differences help tell them apart:
- Asthma pain often comes with wheezing or coughing.
- Heart pain is heavier, sometimes spreading to the arm, back, or jaw.
- Inhalers usually ease asthma pain but they do not help with heart pain.
- Heart pain may cause sweating, nausea, and dizziness.
Warning Signs That Need Quick Medical Attention
You should seek immediate medical help if:
- Chest pain appears suddenly and feels crushing
- Your rescue inhaler is not helping
- Breathing becomes extremely hard
- You feel weak and faint
- Pain occurs after exposure to triggers and does not fade
These could be signs of a serious asthma flare or even a heart issue. If chest pain keeps coming back or feels different than usual, reach out to a healthcare provider.
You can also check online care options like Simple Consult where we let you talk to licensed professionals. Get advice for just $29 with no insurance needed and receive your asthma inhaler prescription refill on the same day.
Conclusion
So, would asthma cause chest pain? Yes, it often does. The pain typically comes from strained respiratory muscles and trapped air that makes your chest feel heavy. In most cases, this signals your asthma needs better management rather than indicating a heart problem.
Still, never assume it is just asthma or a heart issue on your own. Chest pain deserves attention especially if it is unusual and severe. With the right care, you can breathe easier and keep both your lungs and heart healthy.
Frequently Asked Questions
It is rare but severe asthma attacks can trigger cardiac arrest due to very low oxygen levels.
It is because of the inflamed airways and excessive chest muscles activity to help you breathe.
Using your inhaler as prescribed and avoiding triggers are two best possible relievers. They can help ease chest discomfort and reduce pain.










Add comment